The original version of this post (see bottom half) was in relation to the world’s first ever skull and scalp transplant in 2015. I am now updating the post with news of the world’s first African American face transplant in 2019. And the world’s first combined double hand and face transplant in 2021. The first two of these three examples also involved a bonus: brand new scalp hair.
Note that science has now reached a point where taking dangerous immunosuppressants is a lot safer. Moreover, some researchers think that in future we will need minimal to no immunosuppressants. Especially beyond the immediate short-term after surgery.
Make sure to also read my post on the exciting future of allogeneic hair transplants.
First Ever African American Face Transplant in 2019
The world’s first ever face transplant in an African American person (Robert Chelsea) took place in 2019. Later in the year, the news media widely covered his story with amazing after photos. As of 2019, only around 50 face transplants had been performed worldwide.
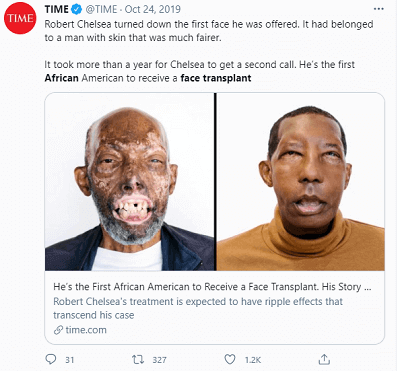
What is also amazing is that 68-year old Mr. Chelsea grew back a young person’s hairline, with dark pigmented hair from the donor face. While this face transplant did not include a full scalp transplant, it seems like a significant portion of the donor scalp was also transferred during the procedure.
10:40 into the below video:
“Now what looks really different is he has hair”.
First Combination Face and Double Arm Transplant in 2021
In 2021, medical and surgical science made yet another big breakthrough. The surgical team from NYU Langone Health performed a face and double hand transplant for 22-year-old Joe DiMeo. Both of these procedures are extremely rare. A combination of the two is quite astounding. The lead surgeon was Dr. Eduardo Rodriguez.
June 4, 2015
In a recent post, I discussed face, organ and limb transplants and the connection with person to person hair transplants. Unlike with organ transplants that save lives, doctors will never prescribe immunosuppressive drugs to those who are bald and want another (dead or alive) person’s hair.
Immunosuppressants are deemed to be too dangerous to be justifiable for any cosmetic procedure. However, I think that people on immunosuppressants rarely seem to die of related causes, especially if they are not that old. Such patients are carefully monitored and dosages are reduced at the slightest signs of any adverse symptoms.
First Ever Skull and Scalp Transplant in 2015

In any event, the reason for writing this post is that earlier today, it was announced that a US surgical team led by Dr. Jesse Selber has performed the world’s first ever skull and scalp transplant on a 55-year-old patient named James Boysen in Texas.
2016 Update: See Jim Boysen’s after photos with significant new scalp hair as a bonus.
For most men in their 50s, needing a haircut is a minor inconvenience. For James Boysen, it’s a nice problem to have.
Within days, his doctors marveled to see the transplanted scalp sweat and his hair grow.
Even more impressive, Mr. Boysen also received a new kidney and a new pancreas during the procedure because his old ones (that were also transplants!!) were failing. Mr. Boysen has had diabetes since age 5, and got his first kidney and pancreas transplants in 1992.
Unfortunately for Mr. Boysen, it seems like the immunosuppressant drugs that he had to take since his original organ transplants in 1992 perhaps contributed to him getting a rare type of cancer called leiomyosarcoma on his scalp in 2006. Although this cancer was treated successfully, it left his scalp significantly damaged. He finally got this scalp transplant after waiting for a donor scalp for a few years.
Mr. Boysen’s perseverance in spite of so much adversity and bad luck are truly admirable. The most interesting part of this story is that Mr. Boysen thinks that the new scalp will give him more hair than he had at age 21. This means that he was extremely bald at a very young age. From his after photo with the new scalp, it seems like the hair on the donor scalp has been shaved, but will grow in the coming months. It will be very interesting to see what Mr. Boysen looks like in another 6 months.
Here is the BBC story of this extraordinary development. My favorite version of this story with a video is on the UK’s Daily Mail. It should be noted that 3D printed skull transplants have been occurring since 2014. Just take a look at this one from this week. But this particular case was the first ever human to human skull transplant.
